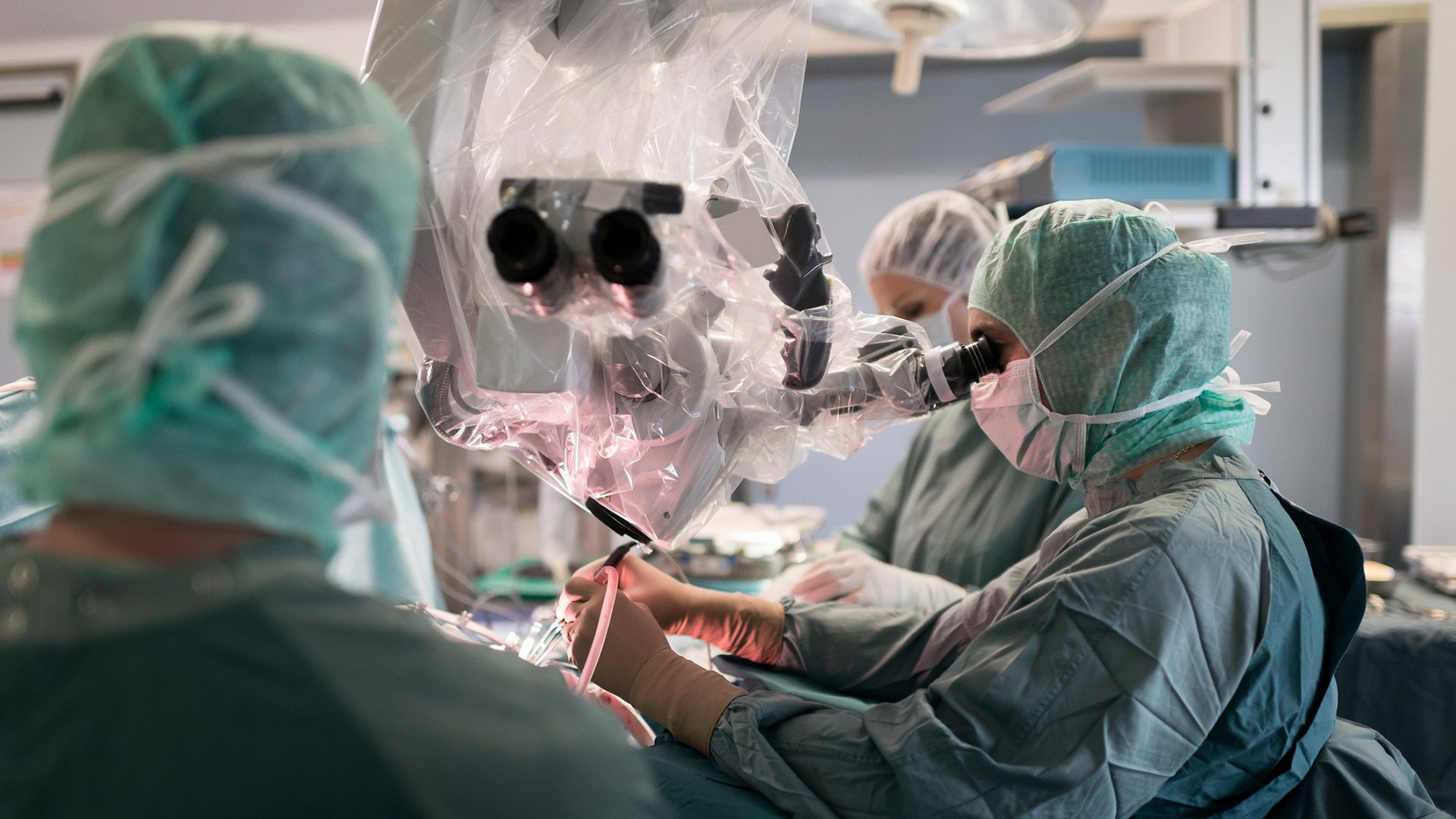
At the Alcor facility in Arizona, more than 150 disembodied heads reportedly lie in cryogenic chambers, preserved in hopes that future medical advances can bring these brains back to life in new bodies. Given that scientists still cannot revive a cryogenically preserved brain, why do patients bother with cryonics at all? Why couldn’t these heads just be stitched onto new bodies in the present day, when they’re still fresh? In other words, why isn’t a brain transplant possible?
Dr. Max Krucoff, an assistant professor of neurosurgery at the Medical College of Wisconsin, would rather describe such a procedure as a body transplant. Unlike a patient who receives a donor heart or liver, transplanting a brain into a patient’s body would make them “a completely new human being,” he told Live Science. “Your agency, your identity, is contained within your brain.”
Sign up for our newsletter
(Image credit: Marilyn Perkins / Future)
Sign up for our weekly Life’s Little Mysteries newsletter to get the latest mysteries before they appear online.
Even a partial brain transplant, such as a cerebellum swap, is out of the question for now. In the case of the cerebellum, the structure is home to millions of specialized neurons called Purkinje cells, each of which receives signals from thousands of other neurons. “The number of connections is exponential,” Krucoff said. “That’s way beyond our capacity.”
Fusing brain and body at the spinal cord would be the simplest theoretical brain transplant, since connections between spinal nerves are more straightforward than neurons in the brain. The surgeon performing this head transplant could connect the skin, muscle, vessels and bones in the neck, and even align the nerves of the spinal cord, “but to get those cells to communicate, we just haven’t figured out how to do that yet,” Krucoff said.
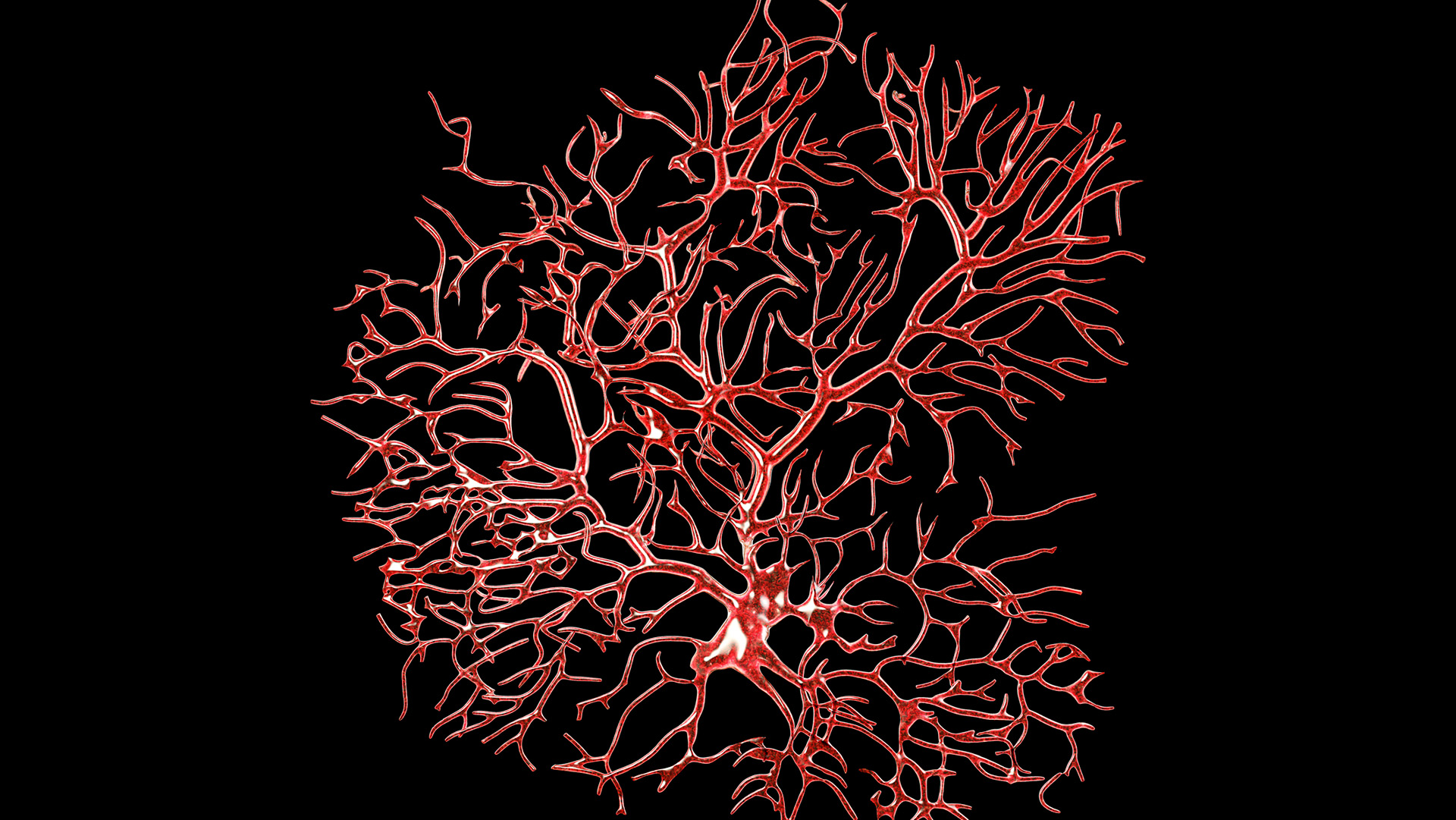
A mass of dendrites branch out from Purkinje cells, receiving signals from surrounding neurons.
(Image credit: KATERYNA KON/SCIENCE PHOTO LIBRARY via Getty Images)
Has a brain transplant ever been attempted?
Scientists began attempting head transplants on animals with the advent of new blood vessel suturing techniques in the early 1900s. Most of the dogs and monkeys involved in those experiments survived a few days at most, as researchers struggled to create a working vascular system or to manage host rejection of the transplanted head with immunosuppressive agents.
Starting in 1970, Dr. Robert J. White transplanted the heads of monkeys onto new host bodies. The animals could chew and swallow food after surgery, and postsurgical electroencephalogram readouts suggested that their brains were awake, though none survived more than nine days.
Inspired by this work, Italian surgeon Dr. Sergio Canavero laid out his vision for the first human head transplant in 2013, attracting widespread pushback from colleagues on ethical and scientific grounds. Canavero’s 2017 announcement that he had performed the first head transplant on a human cadaver was described at the time as “the continuation of a despicable fraud” by New York University bioethicist Arthur Caplan, who pointed out the likelihood of immune rejection and the challenge of linking a brain with all-new nervous inputs.
Can any tissue be transplanted into the central nervous system?
Although a surgeon can’t switch one brain out for another, stem cell or organoid grafts could one day replenish damaged or diseased brain tissue.
Stem cells programmed to develop into neurons may have better odds of integrating into existing circuitry than mature neurons do, said Ruslan Rust, an assistant professor of research physiology and neuroscience at the University of Southern California Keck School of Medicine.
Ideally, these stem cells could be derived from the patient’s own tissue, to lower the odds of immune rejection, but standardized donor cell lines reduce the need for quality control on individual tissue samples. In this way, neurons originating from one person’s tissue could populate another person’s brain.
Stem cell therapies have been tested in clinical trials for Parkinson’s disease, stroke, spinal cord injury and epilepsy, but none of these treatments for these conditions are approved by the U.S. Food and Drug Administration for commercial use.
Rust told Live Science that future research will need to address the potential risks of these techniques, such as incompletely differentiated stem cells forming a tumor after transplant, or cells that do become neurons disrupting signaling pathways.
“The billion dollar question is, how do we make [transplanted cells] the cells that we want them to be, and how do we make sure that they integrate into those local circuitries where we want them to go?” he said.
Stem cells are also used to create lab-grown models of nervous tissues, called organoids, that can be transplanted into the brain. A 2023 study reported that human brain organoids could repair injured rat cortex, though therapies based on organoid transplant are still years away. Rust said such procedures could be more invasive than transplanting individual stem cells, and would need to account for vascular supply to the new tissue.
See how much you know about the most complex organ in the human body with our brain quiz!
TOPICS